Cataracts are a common eye condition that affects many people, particularly as they age. If left untreated, cataracts can significantly impact a person’s quality of life and even lead to blindness. Fortunately, cataract surgery is a highly effective treatment that can restore vision and improve overall well-being.
In this article, we will explore the cataracts surgery experience through real-life stories from patients who have undergone the procedure and regained their vision.
Understanding Cataracts and Their Impact on Vision
What Are Cataracts?
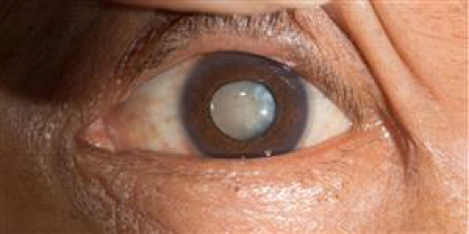
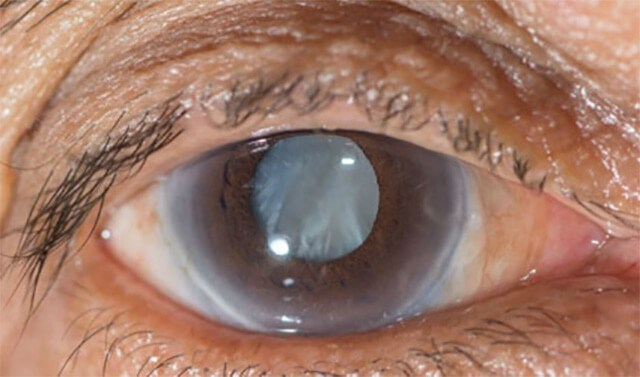
Cataracts are a clouding of the lens in the eye, which can cause blurred vision, sensitivity to light, and other visual disturbances. They typically develop slowly over time and can affect one or both eyes. Cataracts are the leading cause of blindness worldwide, and it is estimated that more than half of the population will have developed cataracts by the age of 80.
Causes and Risk Factors of Cataracts
While cataracts are most commonly associated with aging, they can also be caused by a variety of other factors, such as genetics, injury, and disease. Some of the most common risk factors for cataracts include smoking, diabetes, exposure to UV radiation, and certain medications.
Symptoms and Effects on Daily Life
The symptoms of cataracts can vary depending on the severity of the condition, but they often include blurred or hazy vision, difficulty reading or seeing in low light, and increased sensitivity to glare. These visual disturbances can make it challenging to perform everyday activities such as driving, reading, and watching television.

The Cataract Surgery Process
Preparing for Cataract Surgery
Before undergoing cataract surgery, patients will typically meet with their ophthalmologist for a comprehensive eye exam to assess their vision and overall eye health. During this exam, the doctor will evaluate the patient’s eyes to determine the severity of the cataract and identify any other potential eye conditions that may affect the surgery.
Patients may also undergo a series of tests, including a visual acuity test, a slit-lamp exam, and an ultrasound of the eye to help the doctor plan the surgery. In addition, patients will receive instructions on how to prepare for the procedure, including what medications to avoid and when to stop eating and drinking before the surgery.
It is important for patients to follow these instructions carefully to ensure the best possible outcome from the surgery.
The Procedure: What to Expect
On the day of the procedure, patients will typically arrive at the surgical center or hospital several hours before the surgery is scheduled to begin. This allows time for the patient to complete any necessary paperwork and for the medical staff to prepare the patient for the procedure.
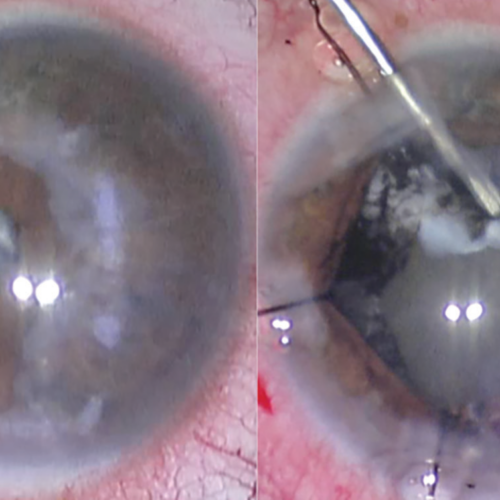
Before the surgery begins, the patient will receive a local anesthetic and sedative to help them relax. The surgeon will then make a small incision in the eye and use a special tool to break up the cloudy lens. They will then use suction to remove the lens fragments and replace it with an artificial intraocular lens.
During the procedure, patients may feel some pressure or discomfort, but this is typically mild and temporary. Most patients are able to return home the same day as the surgery.
Recovery and Post-Operative Care
Following cataract surgery, patients will need to take special care of their eyes to ensure proper healing. This may include applying eye drops, avoiding strenuous activities, and wearing an eye patch or shield at night to protect the eye.
Patients should also avoid rubbing their eyes or getting water in their eyes for several days after the surgery to prevent infection. It is important for patients to attend all follow-up appointments with their doctor to monitor their progress and ensure that their vision is improving.
In most cases, patients experience a significant improvement in their vision within a few days of the surgery. However, it may take several weeks for the eye to fully heal and for the patient to achieve their optimal vision.
Overall, cataract surgery is a safe and effective procedure that can significantly improve a patient’s quality of life. By following their doctor’s instructions and taking proper care of their eyes, patients can enjoy clear vision and a faster recovery after the surgery.

Real-Life Stories of Vision Restoration
As people age, their risk of developing cataracts increases. Cataracts are a clouding of the eye’s natural lens, which can cause vision problems such as blurry vision, sensitivity to light, and difficulty seeing at night. Fortunately, cataract surgery is a safe and effective procedure that can restore vision and improve quality of life. In this article, we will explore real-life stories of patients who have undergone cataract surgery and experienced the benefits of restored vision.
Overcoming Fear and Anxiety
For many people, the idea of undergoing surgery can be intimidating and scary. However, patients who have undergone cataract surgery often report feeling relieved and grateful for the improved vision that the procedure provides. One patient, Susan, shared that she was initially hesitant to undergo surgery but was ultimately glad that she did: “The difference in my vision before and after was remarkable. I can now see clearly and do the things that I love without any hesitation.”
It’s important to note that cataract surgery is a relatively quick and painless procedure that is performed under local anesthesia. The surgeon removes the clouded lens and replaces it with an artificial lens, which can restore clear vision.
The Immediate Impact of Regained Vision
For patients who have been living with cataracts for months or even years, the immediate impact of regained vision can be life-changing. Many patients report feeling more confident and independent, and are able to resume activities that they had previously been unable to do. “I can finally drive again!” exclaimed John, another patient who underwent cataract surgery. “It’s like a weight has been lifted off my shoulders.”
It’s not uncommon for patients to feel a sense of joy and relief after cataract surgery. They may be able to see colors more vividly or read small print without difficulty. These small improvements can have a big impact on their daily lives.
Long-Term Benefits and Lifestyle Changes
In addition to the immediate impact of improved vision, patients who undergo cataract surgery also experience long-term benefits such as a reduced risk of falls and improved cognitive function. Studies have shown that cataract surgery can improve balance and reduce the risk of falls, which is especially important for older adults who may be more prone to falls.
Many patients also report making lifestyle changes such as exercising more frequently and spending more time outdoors now that they have clear vision. With improved vision, patients may be more motivated to engage in physical activity and enjoy the outdoors.
In conclusion, cataract surgery can be a life-changing procedure for patients who are living with vision problems. Patients who undergo the procedure often experience immediate improvements in their vision, as well as long-term benefits such as a reduced risk of falls and improved cognitive function. If you or a loved one is experiencing vision problems due to cataracts, talk to your doctor about the benefits of cataract surgery.

The Role of Technology in Cataract Surgery
Cataract surgery is a common procedure that involves removing the cloudy lens of the eye and replacing it with an artificial lens. While cataract surgery has been performed for centuries, recent advancements in surgical techniques and technologies have made the procedure safer, more precise, and more effective than ever before.
Advancements in Surgical Techniques
One of the most significant advancements in cataract surgery is the use of femtosecond laser technology. This technology allows surgeons to create a precise map of the eye and use the laser to remove the cataract with minimal disruption to the surrounding tissue. This results in faster healing times and improved visual outcomes for patients.
Another advancement in surgical techniques is the use of topical anesthesia, which eliminates the need for injections around the eye. This makes the procedure less invasive and more comfortable for patients.
Intraocular Lens Options
One of the most exciting developments in cataract surgery is the variety of intraocular lens options available to patients. In the past, patients were limited to a single type of artificial lens. However, today’s patients have a range of options to choose from, including multifocal lenses, toric lenses, and accommodating lenses.
Multifocal lenses are designed to provide clear vision at multiple distances, reducing the need for glasses or contact lenses. Toric lenses are designed to correct astigmatism, a common vision problem that can cause blurry or distorted vision. Accommodating lenses are designed to mimic the natural movement of the eye’s lens, providing clear vision at a range of distances.
The Future of Cataract Treatment
While cataract surgery has come a long way in recent years, researchers and medical professionals continue to explore new treatments and technologies to improve patient outcomes. One area of research is gene therapy, which involves using genes to repair or replace damaged cells in the eye. Another area of research is stem cell therapy, which involves using stem cells to regenerate damaged tissue in the eye.
Other potential advancements in cataract treatment include the use of nanotechnology to deliver drugs directly to the eye, and the development of artificial intelligence tools to assist surgeons during the procedure.
Overall, the future of cataract treatment is bright, with new technologies and treatments on the horizon that have the potential to transform the way we treat this common eye condition.
Conclusion
Cataract surgery is a safe and highly effective treatment that can restore vision and significantly improve quality of life for patients. By sharing the experiences of those who have undergone the procedure and highlighting the latest advancements in surgical techniques and technologies, we hope to provide valuable information and insight to those who may be considering cataract surgery.